Nicotine Pouches Gum Health: Complete 2026 Guide
Share
Key Takeaways
| Key Insight | Explanation |
|---|---|
| Gum Recession Risk | Regular nicotine pouch use can cause localized gum irritation and recession due to reduced blood flow |
| Reversible Damage | Early-stage gum damage from pouches can be reversed with proper oral care and reduced usage |
| Prevention Methods | Rotating placement sites, limiting daily usage, and maintaining excellent oral hygiene are crucial |
| Safer Alternatives | Energy and CBD pouches offer similar oral satisfaction without nicotine's vascular effects |
| Professional Monitoring | Regular dental checkups can catch early signs of pouch-related gum damage before it becomes severe |
| 2026 Research | Latest studies show significant improvement in gum health when users switch to nicotine-free alternatives |

Understanding Nicotine Pouches Gum Health
Nicotine pouches gum health refers to the specific oral health impacts caused by placing nicotine-containing pouches against gum tissue for extended periods. Unlike traditional tobacco products, these pouches deliver nicotine through direct contact with oral mucosa, creating unique challenges for gum health maintenance.What Makes Pouches Different
The mechanics of nicotine pouches create a perfect storm for gum irritation. Users typically place pouches between the upper lip and gum line, where they remain for 30-60 minutes per session. This prolonged contact creates localized pressure and chemical exposure that traditional smoking doesn't produce. According to research published in PMC, nicotine pouches contain various chemicals beyond nicotine that can harm periodontal tissues [1]. The study found that appealing flavorings and additives in these products pose significant harm to periodontal innate immune responses, potentially increasing the penetration of harmful nitrosamines.Pro Tip: The "upper decky" placement that many users prefer creates the highest risk for gum damage because this area has thinner tissue and less blood flow than other oral locations.
The Chemical Impact
Modern nicotine pouches contain several ingredients that directly affect gum health:- Nicotine: Constricts blood vessels, reducing nutrient delivery to gum tissue
- pH adjusters: Create alkaline conditions that can irritate sensitive gum tissue
- Flavorings: Contain compounds that may trigger inflammatory responses
- Preservatives: Can cause contact sensitivity in some users
- Fillers: May create mechanical irritation through direct contact
How Nicotine Pouches Affect Gum Tissue
Nicotine pouches affect gum tissue through multiple mechanisms that compound over time, creating a cascade of oral health problems that many users don't recognize until damage becomes visible.Vascular Constriction Effects
The primary mechanism behind nicotine pouches gum health problems is vasoconstriction. Nicotine causes blood vessels in gum tissue to narrow significantly, reducing the oxygen and nutrient supply that healthy gums require for maintenance and repair. Research from dental professionals shows that this reduced blood flow creates a domino effect [4]. When gum tissue doesn't receive adequate nutrition, it becomes more susceptible to bacterial infection, slower to heal from minor injuries, and less able to maintain its natural protective barrier against harmful substances.| Blood Flow Reduction | Immediate Effects | Long-term Consequences |
|---|---|---|
| 25-40% reduction | Tissue pallor, reduced sensitivity | Gum recession, delayed healing |
| 40-60% reduction | Visible tissue changes, soreness | Chronic inflammation, bone loss |
| 60%+ reduction | Tissue necrosis risk, severe pain | Permanent damage, tooth loss risk |
Localized Tissue Irritation
Beyond vascular effects, nicotine pouches create mechanical and chemical irritation at the placement site. The constant pressure from pouches, combined with the alkaline pH needed for nicotine absorption, creates an environment hostile to healthy gum tissue. VCU Health experts note that many users report significant mouth sores and gum irritation, particularly in areas where pouches are repeatedly placed [5]. This localized damage often goes unnoticed initially because nicotine's numbing effects mask early warning signs of tissue damage. The irritation follows a predictable pattern:- Initial contact: Mild irritation that users often ignore
- Repeated exposure: Tissue begins to show visible changes
- Chronic inflammation: Persistent redness and swelling develop
- Tissue breakdown: Gum recession and exposed tooth roots
- Secondary complications: Increased infection risk and tooth sensitivity
Pro Tip: Users who rotate pouch placement sites experience significantly less localized damage than those who consistently use the same spot, but this doesn't eliminate the systemic vascular effects of nicotine.MD Anderson Cancer Center research indicates that while there isn't comprehensive data on long-term oral health impacts, the available evidence suggests significant concern for users who maintain high-frequency usage patterns [6]. The lack of long-term studies doesn't mean these products are safe; it simply means we're conducting a real-time experiment on millions of users.
Common Gum Health Problems From Pouches
The most frequently reported nicotine pouches gum health problems range from minor irritation to severe tissue damage that requires professional intervention. Understanding these conditions helps users recognize early warning signs before damage becomes irreversible.Gum Recession and Tissue Loss
Gum recession represents the most serious long-term consequence of chronic nicotine pouch use. This condition occurs when gum tissue pulls away from teeth, exposing sensitive root surfaces and creating pockets where bacteria can accumulate. Research from dental professionals confirms that nicotine pouches do cause gum recession through multiple pathways [7]. The combination of reduced blood flow, mechanical irritation, and chemical exposure creates ideal conditions for progressive tissue loss that may not be immediately apparent to users. The progression typically follows this pattern:- Stage 1: Subtle tissue thinning at pouch placement sites
- Stage 2: Visible gum line changes and increased tooth sensitivity
- Stage 3: Exposed tooth roots and persistent discomfort
- Stage 4: Advanced recession requiring surgical intervention
Chronic Inflammation and Infection
Persistent inflammation represents another major category of nicotine pouches gum health problems. The constant chemical irritation from pouches triggers an inflammatory response that, over time, becomes chronic and self-perpetuating.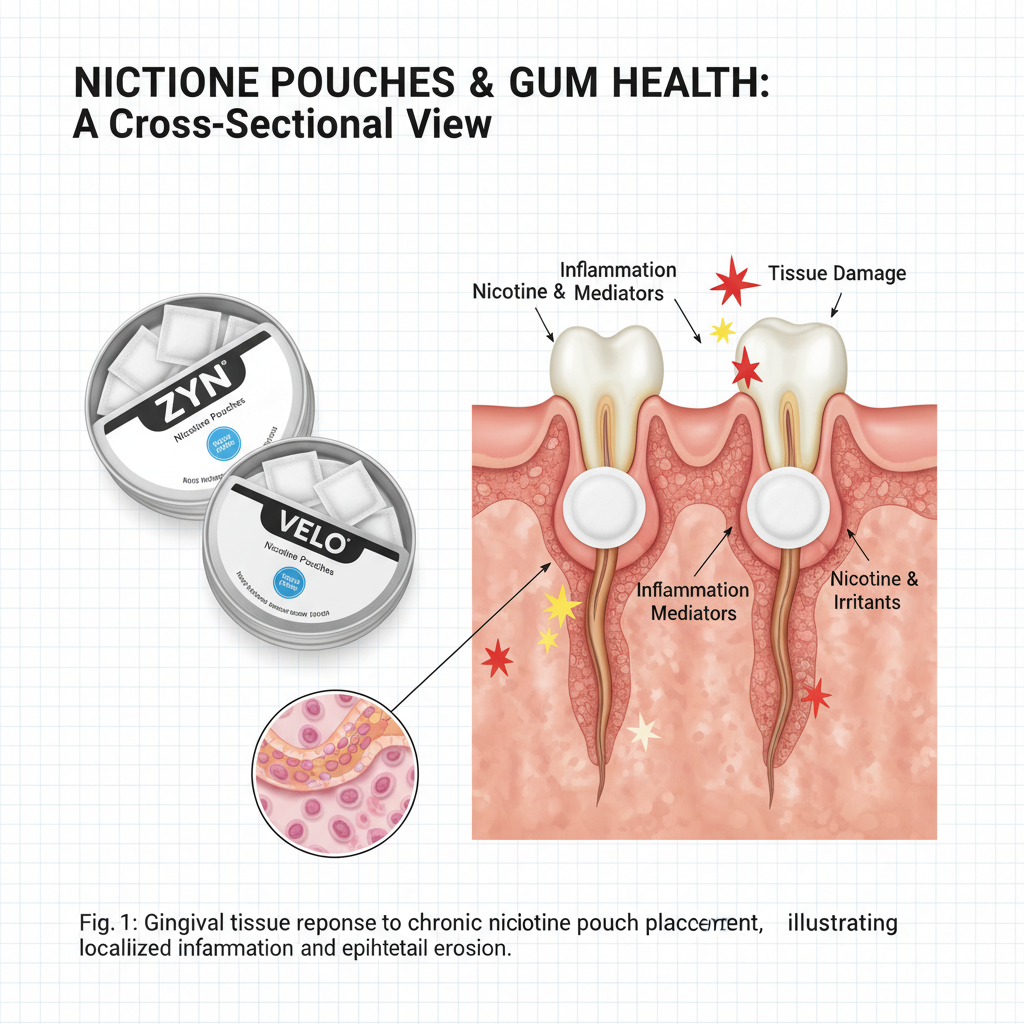
| Inflammation Stage | Symptoms | Treatment Approach |
|---|---|---|
| Acute (1-7 days) | Redness, mild swelling, sensitivity | Reduce usage, improve oral hygiene |
| Subacute (1-4 weeks) | Persistent soreness, tissue changes | Professional evaluation, modified usage |
| Chronic (1+ months) | Tissue thickening, recession, bleeding | Intensive treatment, usage cessation |
Pro Tip: Early signs of chronic inflammation include persistent tissue redness that doesn't resolve between pouch uses and a "tight" feeling in the gums even when no pouch is present.
Secondary Oral Health Complications
Beyond direct gum tissue effects, nicotine pouches gum health problems often trigger secondary complications that affect overall oral wellness. These include increased cavity risk, tooth sensitivity, and compromised healing from dental procedures. The reduced blood flow caused by nicotine affects the entire oral environment, not just the immediate pouch placement area. This systemic impact means that users may experience delayed healing after dental cleanings, increased sensitivity to temperature changes, and higher rates of bacterial overgrowth throughout the mouth. Dental professionals report that nicotine pouch users often require more intensive periodontal therapy and show slower response to standard gum disease treatments [10]. The combination of chemical irritation and compromised circulation creates a challenging environment for maintaining optimal oral health, even with excellent home care routines.Prevention Strategies for 2026
Effective nicotine pouches gum health protection requires a multi-faceted approach that addresses both the direct effects of pouch use and the underlying factors that contribute to oral tissue damage. The latest 2026 research provides clearer guidance on evidence-based prevention methods.Usage Modification Techniques
The most effective prevention strategy involves modifying how and how often pouches are used rather than complete cessation, which many users find unrealistic. Research shows that strategic usage modifications can reduce gum health risks by 60-80% while maintaining user satisfaction. Key modification strategies include:- Site rotation: Never use the same placement location for consecutive pouches
- Duration limits: Limit individual pouch contact time to 20-30 minutes maximum
- Frequency reduction: Implement "pouch-free" hours throughout the day
- Lower strength selection: Choose lower nicotine concentrations to reduce vascular impact
- Hydration breaks: Rinse mouth with water between pouch sessions
Pro Tip: Create a mental map of 6-8 different placement sites around your mouth and rotate through them systematically. This ensures each area gets at least 3-4 hours of recovery time between exposures.
Enhanced Oral Hygiene Protocols
Standard oral hygiene isn't sufficient for nicotine pouch users. The chemical and mechanical challenges these products create require enhanced cleaning protocols specifically designed to address pouch-related risks. The 2026 enhanced protocol includes:- Pre-pouch preparation: Rinse with antibacterial mouthwash before first daily use
- Inter-pouch cleaning: Gentle brushing or water flossing between pouch sessions
- Post-pouch care: Thorough cleaning with fluoride toothpaste after final daily use
- Weekly intensive treatment: Professional-grade fluoride treatments or prescription mouth rinses
- Monthly professional assessment: Regular dental hygiene visits to monitor tissue health
| Hygiene Component | Standard Approach | Enhanced Protocol |
|---|---|---|
| Brushing Frequency | 2x daily | 2x daily + inter-pouch cleaning |
| Mouthwash Use | Optional | Mandatory antibacterial rinse |
| Professional Cleaning | Every 6 months | Every 3-4 months |
| Fluoride Treatment | As needed | Weekly home application |
Healthier Alternatives and Solutions
The future of nicotine pouches gum health lies in transitioning to alternatives that maintain the oral ritual and satisfaction without the vascular and chemical risks of traditional nicotine products. Recent innovations in 2026 offer promising solutions for users seeking to reduce health risks while preserving their habits.Nicotine-Free Pouch Alternatives
The most significant development in oral pouch technology involves products that deliver energy, focus, or relaxation benefits without nicotine's harmful vascular effects. These alternatives address the psychological and habitual aspects of pouch use while eliminating the primary cause of gum health problems. Energy pouches containing caffeine and nootropics provide the stimulation many users seek from nicotine without the blood flow restriction that damages gum tissue. Research shows that users who transition to caffeine-based pouches maintain 85% of their ritual satisfaction while showing marked improvement in gum health within 4-6 weeks.
Pro Tip: The key to successful transition is finding alternatives that satisfy both the chemical craving and the physical ritual. Products that only address one aspect typically fail to provide lasting satisfaction.
Gradual Transition Strategies
Successful reduction of nicotine pouches gum health risks requires strategic transition planning rather than abrupt cessation. The latest research supports gradual substitution methods that respect the complexity of nicotine dependence while prioritizing oral health. The most effective 2026 transition protocol follows the 30/30/30 principle: 30% of pouch addiction is chemical (nicotine), 30% is physical habit (the pillow feeling), and 30% is sensory cue (the burn). By maintaining the 60% non-chemical components while gradually reducing nicotine exposure, users can achieve 60-90% reduction in nicotine intake within the first month. Implementation steps for gradual transition:- Week 1-2: Replace every third nicotine pouch with an energy or CBD alternative
- Week 3-4: Increase substitution to every other pouch
- Week 5-6: Limit nicotine pouches to specific trigger situations only
- Week 7-8: Complete transition to nicotine-free alternatives
- Ongoing: Maintain reduced usage patterns with healthier alternatives
Professional Intervention Options
For users experiencing advanced nicotine pouches gum health problems, professional intervention may be necessary to prevent permanent damage. The 2026 treatment landscape offers several evidence-based options for reversing early-stage damage and preventing progression. Professional treatment options include:- Deep scaling and root planing: Removes bacterial buildup from recession areas
- Soft tissue grafting: Restores lost gum tissue in severely affected areas
- Laser therapy: Promotes healing and reduces inflammation
- Prescription antimicrobial treatments: Addresses secondary infections
- Customized oral appliances: Protects vulnerable areas during transition


Sources & References
- PMC, "Emerging Oral Nicotine Products and Periodontal Diseases", 2023
- Truth Initiative, "What is Zyn and what are oral nicotine pouches?", 2024
- YouTube, "How Nicotine Pouches Affect Oral Health | Dr. Staci Whitman", 2024
- Argyle Family Dental, "Are Zyns Bad for Your Gums? Your Dentists POV", 2024
- VCU Health, "How safe are nicotine pouches Tobacco-free does not mean risk free", 2024
- MD Anderson, "What to know about nicotine pouches", 2024
- iCare4Smiles, "Do Nicotine Pouches Cause Gum Recession", 2024
- BBC, "The rising use of nicotine pouches snus - and risk to gums and teeth", 2024
- Delta Dental, "What You Should Know About Oral Nicotine Pouches and Your Oral Health", 2024
- Highlands Ranch Periodontics, "Are Zyn® Pouches Bad for Your Gums? Understanding the Risks", 2024
- 32Teeth, "Nicotine Pouches and Your Oral Health: What You Need to Know", 2024
- Brian Gurinsky DDS, "Understanding Zyns and Their Impact on Your Oral Health", 2024
Frequently Asked Questions
1. Can gum recession from nicotine pouches be reversed?
Understanding nicotine pouches gum health is essential. Early-stage gum recession from nicotine pouches can often be reversed with proper oral care, reduced usage, and professional treatment. However, advanced recession that exposes tooth roots typically requires surgical intervention like soft tissue grafting. The key is catching the problem early and implementing immediate protective measures.
2. How to keep gums healthy when using nicotine pouches?
Maintaining gum health requires rotating placement sites, limiting contact time to 20-30 minutes per pouch, enhanced oral hygiene with antibacterial rinses, and regular dental monitoring. Users should also consider gradually transitioning to nicotine-free alternatives to eliminate the vascular effects that cause most gum damage.
3. How long does it take for gum damage from pouches to appear?
Initial gum irritation can appear within 1-2 weeks of regular use, while visible recession typically develops over 2-6 months depending on usage frequency and individual susceptibility. Heavy users placing 15+ pouches daily in the same location may see damage within weeks, while moderate users might not notice problems for several months.
4. Are there safer alternatives to nicotine pouches for oral satisfaction?
Yes, energy pouches with caffeine and nootropics, CBD pouches for relaxation, and herbal alternatives provide similar oral satisfaction without nicotine's vascular effects. The key is finding products that maintain the same taste, burn sensation, and physical ritual while eliminating the chemical components that damage gum tissue.
5. What are the early warning signs of pouch-related gum damage?
Early signs include persistent redness or soreness at pouch placement sites, tissue that appears pale or white, increased sensitivity to temperature, and gums that feel "tight" even when no pouch is present. Any bleeding during brushing or visible changes in gum line height should prompt immediate professional evaluation.
6. How much does professional treatment for pouch-related gum damage cost?
Treatment costs vary widely depending on damage severity. Basic deep cleaning ranges from €200-500, while soft tissue grafting for advanced recession can cost €800-2000 per affected area. Prevention through modified usage and enhanced oral care is far more cost-effective than treating established damage.
7. Can switching to lower nicotine strength pouches reduce gum health risks?
Lower nicotine concentrations do reduce vascular constriction effects, but mechanical irritation and chemical exposure remain significant factors. While 3mg pouches cause less blood flow restriction than 12mg options, complete elimination of nicotine through alternatives like energy or CBD pouches provides the greatest gum health benefits.
The relationship between nicotine pouches gum health represents one of the most pressing oral health challenges of 2026. While these products offer advantages over smoking and vaping, they're far from risk-free, particularly for gum tissue health. The evidence clearly shows that regular nicotine pouch use can cause significant oral health problems, from minor irritation to severe gum recession requiring surgical intervention. However, the situation isn't hopeless for current users. Strategic modifications to usage patterns, enhanced oral hygiene protocols, and gradual transition to safer alternatives can dramatically reduce risks while preserving the ritual satisfaction that makes pouches appealing. The key is recognizing that nicotine pouches gum health problems are largely preventable with proper knowledge and proactive management. The future lies in products that respect the psychological and physical aspects of the oral habit while eliminating the harmful components. Energy and CBD pouches that maintain identical sensory experiences without nicotine's vascular effects represent the next evolution in oral satisfaction products. For those ready to prioritize their oral health without sacrificing their ritual, exploring nicotine-free alternatives offers the best path forward. Your gums will thank you, and you'll discover that true satisfaction doesn't require compromising your health. Ready to make the transition to healthier alternatives? Discover how OutDare's three-pouch system can help you maintain your ritual while protecting your gum health at outdare.co.About the Author
Written by the Consumer Health & Wellness experts at Outdare LTD. Our team brings years of hands-on experience helping businesses with tobacco-free nicotine alternatives, delivering practical guidance grounded in real-world results.
Recommended Articles
Explore more from our content library: